DEPARTMENTS
BY THE NUMBERS
Opioid Abuse and Workers’ Compensation
In December, CDC released a guideline for public comment regarding the prescription of opioids for treating chronic pain. Statistics indicate a 200 percent increase since 2000 in fatal overdoses attributable to opioids (including heroin and prescription medications) in the United States. Since opioids are often prescribed through workers’ compensation programs, NIOSH has requested suggestions for additional resources for its Center for Workers’ Compensation Studies.
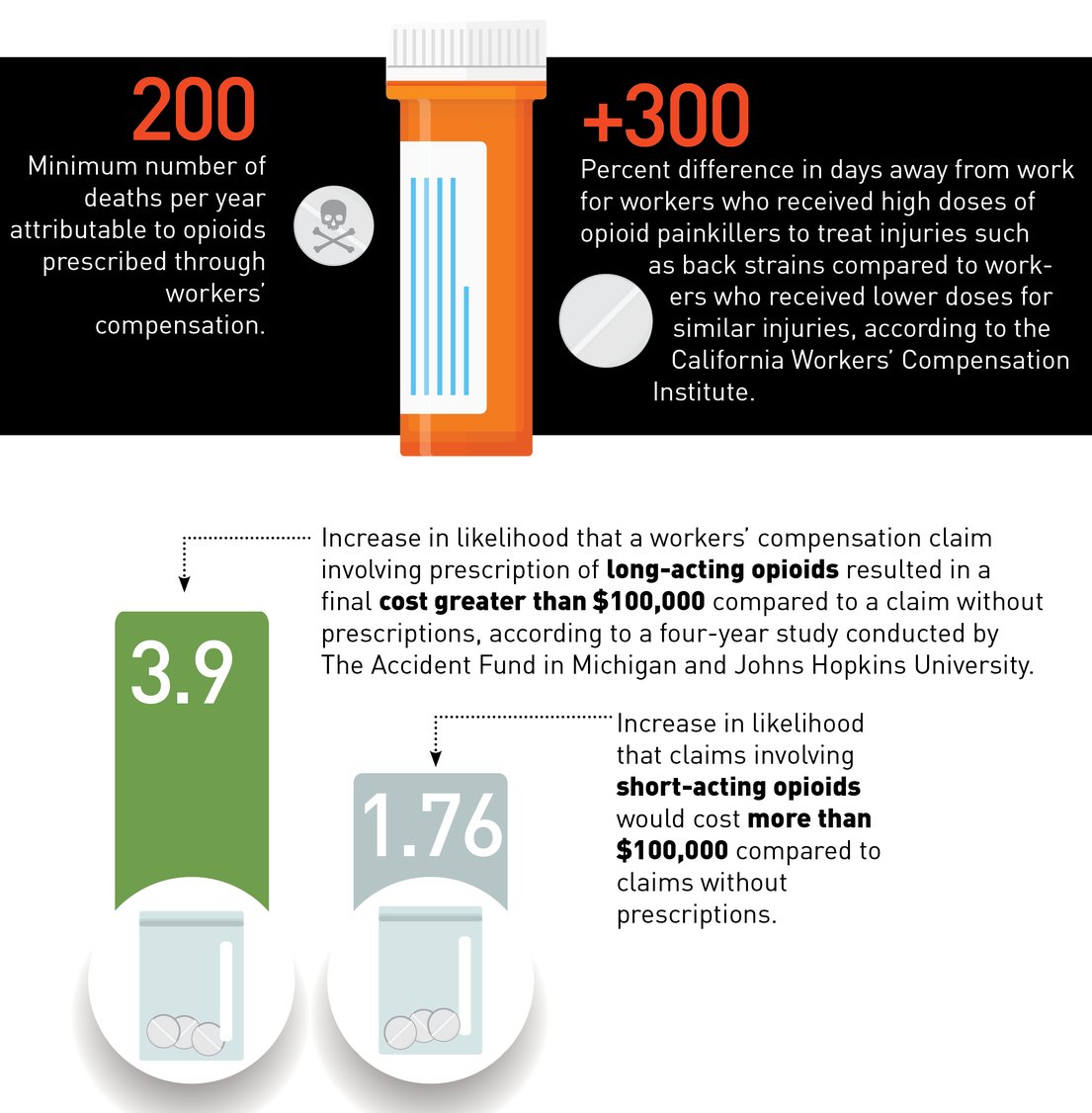
The information below appears in a 2013 report from the International Association of Industrial Accident Boards and Commissions titled “Reducing Inappropriate Opioid Use in Treatment of Injured Workers: A Policy Guide.” The report summarizes recent research on the use of opioid prescription drugs in workers’ compensation systems and suggests several public policy responses.
SOURCES
CDC: Draft CDC Guideline for Prescribing Opioids for Chronic Pain (December 2015).
International Association of Industrial Accident Boards and Commissions: “Reducing Inappropriate Opioid Use in Treatment of Injured Workers: A Policy Guide” (PDF, August 2013).
NIOSH Science Blog: “The Opioid Overdose Epidemic and the Workplace” (December 2015).
From the NIOSH Science Blog:
“The use of prescription opioids may impact the ability of a person to return to work, and ultimately can negatively affect their livelihood. If workers are under the influence of opioids while they are at work, they are likely to be at increased risk for injury. For workers in safety sensitive jobs, such as transportation and operators of heavy equipment, there will be increased risks for catastrophic events that impact many besides the worker.”
thesynergist | TOC | NEWSWATCH | DEPARTMENTS | COMMUNITY
Editor's Note: Fumes vs. Vapors
The original wording from the Center for Public Integrity's report "Common Solvent Keeps Killing Workers, Consumers" mistakenly refers to "fumes" in a context where "vapors" is the correct term. The Synergist has corrected this error in the digital edition.
Unfortunately, the error found its way into the print version of the November issue. The Synergist regrets the error and will publish a correction in the December issue.
Ed Rutkowski, editor

